Volume 3, Issue 12
December 2023
Orthopedic Complications in Diabetes: Charcot Foot, Neuropathy, and Surgical Considerations
Abdullah Aborukbah, Faisal Alghamdi, Hisham Elbashir, Abdulaziz Alghamdi, Ahmed Alzahrani, Mohammed Alghamdi, Saber Baseem, Fahad Almalki, Manar Shehata, Mohanad Alkindy, Marwan Algaidi
DOI: http://dx.doi.org/10.52533/JOHS.2023.31223
Keywords: Orthopedic Complications, Diabetes Mellitus, Charcot Foot, Diabetic Neuropathy, Surgical Management
Orthopedic problems in individuals with diabetes are complex and challenging to handle. Among these issues, Charcot foot stands out as a debilitating condition characterized by joint destruction and deformities. This condition is closely linked to neuropathy and inflammation, leading to bone weakening and joint damage. Unfortunately, Charcot foot often goes unnoticed until significant complications arise, underscoring the importance of recognition and intervention. Diabetic neuropathy, affecting around half of all people with diabetes, further complicates challenges by causing loss, autonomic dysfunction and muscle weakness. Sensory loss in the feet puts individuals at risk for injuries, ulcers, and other complications. The diverse symptoms associated with neuropathy impact patients daily. Require individualized management strategies. Surgical considerations in patients add a layer of complexity to their care. Thorough preoperative assessments, infection control measures, vascular evaluations and careful postoperative monitoring are crucial for surgical management. Collaboration among healthcare professionals from specialties is vital for optimizing outcomes. Effective management strategies for these complications involve offloading pressure on affected areas to prevent injury or trauma, maintaining tight glycemic control to minimize complications, providing pain relief to alleviate discomforts experienced by patients and implementing rehabilitation programs that enhance functionality. It is crucial to prioritize identification, prompt intervention, and thorough patient education to achieve results and enhance the overall well-being of individuals with diabetes. To summarize, managing orthopedic issues in patients necessitates a comprehensive strategy that takes into account the complexities of Charcot foot diabetic neuropathy and surgical treatments.
Introduction
Diabetes mellitus, a metabolic disorder is closely linked to several orthopedic complications, including Charcot foot, neuropathy and specific surgical challenges (1). These complications primarily arise from the long-term effects of blood sugar levels, which cause changes in the body’s neurovascular and biomechanical aspects. To effectively provide care to individuals, with diabetes it is essential to have an understanding of the complexities involved including their underlying mechanisms and suitable management strategies (2, 3). Charcot foot or neuropathic osteoarthropathy is one of the orthopedic issues associated with diabetes. Although not as prevalent as complications it poses a significant risk due to its debilitating consequences. The development of Charcot foot involves a combination of neuropathy that impairs autonomic functions and an abnormal inflammatory response (4). This leads to bone demineralization and joint damage exacerbated by injuries that go unnoticed due to diminished sensation. Studies have demonstrated that these factors contribute to bone and joint destruction that can ultimately result in deformities, ulcers and in severe cases amputation (5, 6). Peripheral neuropathy contributes to the development of these issues, in individuals with diabetes. Around half of individuals with diabetes will encounter a type of nerve damage known as neuropathy (7, 8). The risk of developing neuropathy is higher for those who have had diabetes, for a duration or have maintained controlled blood sugar levels. The loss of feeling is a factor, in the development of foot sores and subsequent complications like infections and Charcot foot (9, 10). Managing patients through surgery presents challenges. Diabetic individuals, those with nerve problems or circulation issues face a higher risk of postoperative complications such as infections, delayed wound healing and poor bone recovery. A study highlighted these risks. It is crucial to highlight the significance of managing blood sugar levels both before and after surgery. To achieve the surgical results a cooperative approach involving surgeons, endocrinologists, podiatrists, and wound care specialists is essential. The management strategies for complications in patients are diverse and should be customized to each person’s unique needs. In cases of Charcot foot, early recognition and management play a role (11). Conservative approaches often involve immobilization and offloading to prevent harm and promote healing. Surgical intervention might be necessary if there is deformity or instability present. Another study emphasized the significance of footwear and orthotics in preventing sores and deformities in individuals with Charcot foot. For neuropathy the focus is on controlling blood sugar levels to prevent or slow down nerve damage progression. Effective pain management is also crucial, which may include medications like antidepressants, anticonvulsants or topical treatments. Different research conducted an analysis of the medical and non-medical approaches to treating neuropathic pain in individuals with diabetes. They highlighted the importance of educating patients. Consistently monitoring their condition as aspects of successfully managing neuropathy. When it comes to patients it's crucial to assess their vascular status and potential infection risks before surgery. During the operation surgeons need to use techniques and aftercare should include monitoring for signs of infection and ensuring wound healing. In the study comprehensive guidelines were outlined for managing complications related to diabetic foot problems. These guidelines highlight the importance of care plans and the collaboration of a team in achieving successful surgical outcomes. This review aims to examine complications associated with diabetes, such as Charcot foot and neuropathy along, with the considerations that need to be taken when performing surgery.
Discussion
Orthopedic issues related to diabetes challenges, in patient care. One such complication, known as Charcot foot, is a severe condition that arises from peripheral neuropathy and an abnormal inflammatory response. This condition can cause deformities and ulcers highlighting the importance of detection and proper management. Diabetic neuropathy, which affects half of individuals with diabetes manifests as autonomic and motor neuropathies. It leads to loss, autonomic dysfunction and muscle weakness (12). Various elements play a role in the formation of foot ulcers and the subsequent complications that may arise from them. When it comes to interventions for patients a thorough preoperative assessment is essential along with infection control measures, vascular evaluation procedures and postoperative monitoring (13, 14). Taking an approach is crucial for achieving outcomes in these cases.
Clinical Manifestation
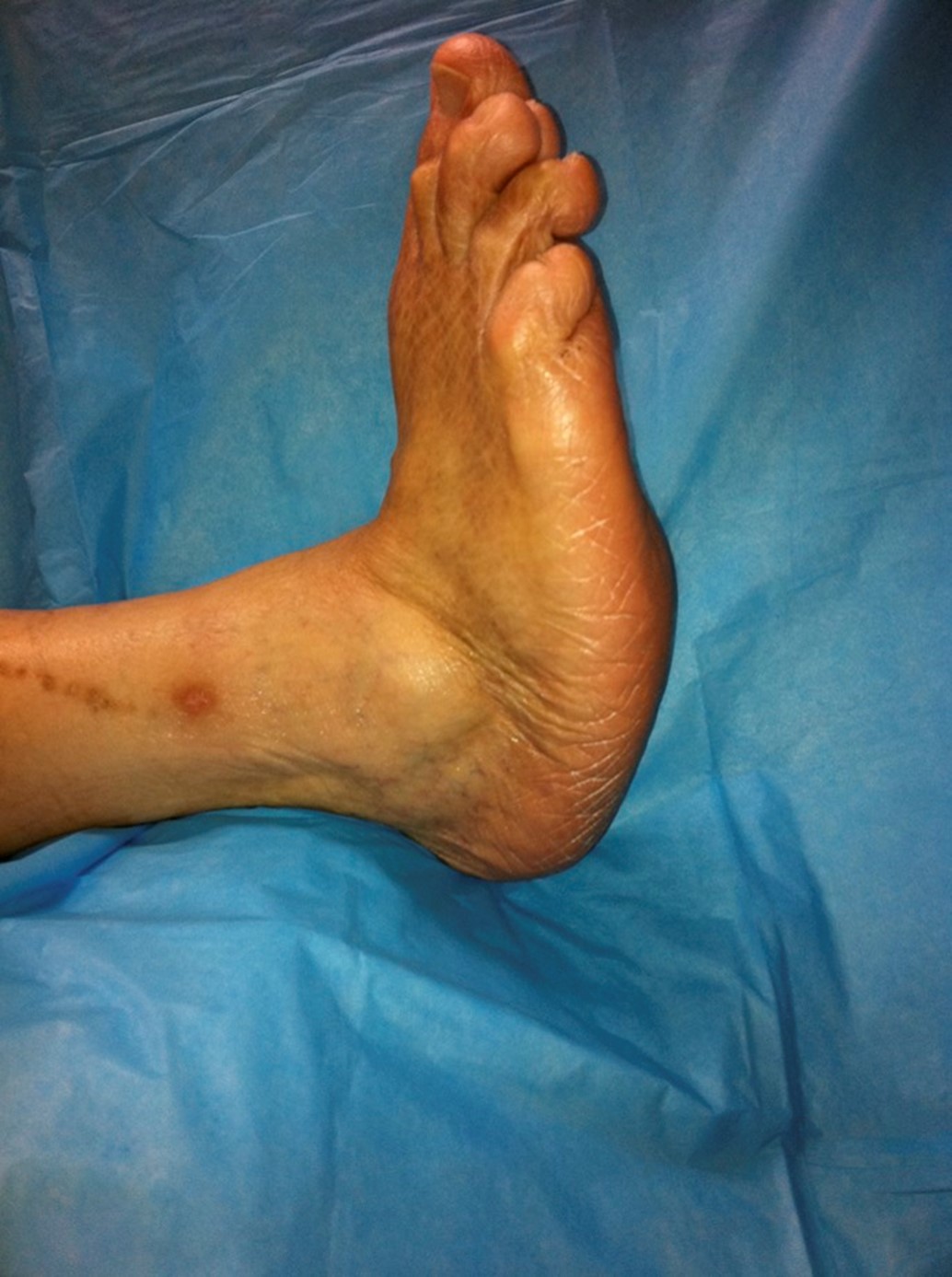
Orthopedic issues associated with diabetes can present in ways, such, as the development of Charcot foot, nerve damage and the need to consider options (15). Complications such as charcot foot, neuropathy and surgical considerations can arise due to the interactions between diabetes related changes in the body (Figure 1). These complications often present as scenarios that require careful evaluation and management.

Figure 1: The typical appearance of a later-stage Charcot foot with a rocker-bottom deformity (1).
Charcot foot, which is also known as osteoarthropathy exemplifies the nature of orthopedic issues in diabetes. This condition typically begins with localized swelling and redness which can resemble signs of infection. The affected area may have increased skin temperature due to a response. Improved blood flow caused by minor injuries. Interestingly Charcot foot is characterized by the absence of pain when fractures or joint dislocations are present (16). As the condition progresses deformities may develop over time causing changes in the structure and function of the foot. These deformities often lead to ulceration—a consequence of neuropathy—as patients lose their ability to sense pressure or injury. Instability and limited mobility further complicate matters and impact a patient’s overall quality of life. Diabetic neuropathy, a debilitating complication of diabetes manifests in ways with distinct clinical manifestations. Peripheral neuropathy is the form and primarily affects sensory function. Patients frequently report disturbances in their extremities such as numbness and tingling sensations. However, one of the characteristics of neuropathy is the decreased ability to feel sensations, which puts patients at risk, for injuries especially in their feet. This diminished sensation makes individuals more prone to developing ulcers and experiencing complications related to trauma (17). Autonomic neuropathy, which is a component of neuropathy, presents a range of clinical manifestations that go beyond the peripheral nerves. Gastrointestinal symptoms, like gastroparesis cardiovascular problems such as hypotension and genitourinary issues like dysfunction can all occur due to autonomic neuropathy (18). These manifestations greatly affect patient’s lives and necessitate specific care and management. Motor neuropathy, although less common, also contributes to the spectrum of neuropathy. This type of neuropathy can lead to muscle weakness affecting patients’ balance and coordination. The weakness and motor impairments experienced by individuals with motor neuropathy further increase the risk of falls and injuries (19). When dealing with patients who have issues it is important to evaluate and manage a range of factors. Poor wound healing is a manifestation that can result in healing ulcers or surgical incisions becoming chronic and problematic. Diabetic patients also face an increased risk of infections, which may present with localized redness, swelling, warmth or purulent discharge as signs. The insidious nature of neuropathy can lead to the development of ulcerations after surgery that often go unnoticed until complications arise. Surgical procedures on the extremities are particularly prone to complications such as delayed fracture healing and vascular issues. These symptoms can appear as refill weakened pulses and changes, in skin color (20). It is crucial to keep an eye on these indicators and promptly take measures. Diabetes can lead to complications such, as Charcot foot, surgical issues. It is crucial for healthcare practitioners to possess the ability to recognize these complications in order to take action and prevent outcomes such as limb amputation or disability. It is of importance to closely monitor patients for these complications in order to provide them with quality care and achieve favorable results. Having an understanding of these manifestations is essential for providing effective treatment, to this vulnerable group of patients.
Management
Managing orthopedic complications in patients with diabetes is an aspect of healthcare especially when dealing with conditions, like Charcot foot, neuropathy and surgical considerations. It is essential to take an approach to handle these complications effectively, improving outcomes and reducing the risks associated with diabetes.
Charcot Foot Management
Charcot foot, which is also known as neuropathic osteoarthropathy presents challenges when it comes to treatment. The main goals of managing this condition are to reduce inflammation, stabilize the foot, prevent deformities and promote healing of any wounds. One key strategy in Charcot foot management involves offloading and immobilizing the foot. This helps prevent injury to the area. Total contact casting (TCC) is a used technique that effectively redistributes pressure away from the part of the foot. Additionally, customized footwear orthotics and bracing can provide support and offloading. In order to manage inflammation and pain during the phase doctors may prescribe inflammatory medications like non-steroidal anti-inflammatory drugs (NSAIDs). However, caution should be exercised when considering their use in patients with kidney problems or contraindications. Maintaining control over blood sugar levels is an aspect of Charcot foot management. It's important to keep blood glucose levels optimal in order to minimize complications and facilitate healing overall. Regular monitoring of blood sugar levels and appropriate adjustments to insulin or oral antidiabetic medications are components of maintaining control. Physical therapy plays a role in managing Charcot foot by focusing on restoring strength, balance and mobility, in the limb. Therapists closely collaborate with patients to help improve their abilities while minimizing the chances of injury. In situations where there are deformities or instability surgical intervention might be necessary. Surgeries, like realignment, arthrodesis or osteotomy are performed to correct abnormalities and enhance the overall stability of the affected foot. Taking care of wounds in a manner is an aspect of managing Charcot foot since there is a high incidence of ulceration, in such cases. Regularly cleaning the wounds using dressings and ensuring infection control are parts of wound management.
Diabetic Neuropathy Management
Diabetic neuropathy, a complication of diabetes necessitates an approach to its management. The main goals are to alleviate symptoms, prevent complications and improve the quality of life for patients. Pain management is an aspect in dealing with neuropathy (21, 22). Physicians often prescribe medications such as antidepressants and anticonvulsants to alleviate pain. Opioids are typically avoided due to their nature. Educating patients on foot care practices is essential in managing loss. Regular foot inspections and the use of footwear are preventive measures against injuries and ulcers in patients with reduced sensation. When it comes to autonomic neuropathy specific strategies are employed based on the symptoms experienced by each patient. Dietary changes may be recommended for symptoms while managing blood pressure is crucial for addressing hypotension. For symptoms specialized interventions like medication for dysfunction can be considered if necessary. It is crucial to keep your blood glucose levels at a range as it plays a role in slowing down the advancement of neuropathy and safeguarding against nerve damage. Achieving control requires monitoring of blood glucose levels and adjustments to insulin or oral antidiabetic medications as required. Physical rehabilitation programs play a role in managing diabetic neuropathy by focusing on enhancing muscle strength, coordination, balance improvement and reducing the risk of falls and injuries.
Surgical Considerations Management
During procedures, there are interventions implemented to address the requirements of patients and reduce potential risks ultimately aiming to achieve optimal surgical outcomes. Before any procedure, it is crucial to conduct assessments. These assessments include evaluating the patient’s health, cardiac function and blood sugar control. It is important to address any identified issues before surgery to reduce complications. We also take measures to prevent site infections by administering antibiotics before surgery following aseptic techniques and providing diligent wound care. Assessing health is an aspect of surgical considerations. This helps us identify any blood flow problems that could impact wound healing. If we detect any issues, we may need to involve surgeons or consider vascular interventions. Additionally, continuous monitoring after surgery is vital in order to catch signs of infection delayed wound healing or other complications. Some patients may require hospital stays or frequent outpatient visits for postoperative care. Rehabilitation programs such as occupational therapy play a role in helping patients regain mobility and functionality for their overall recovery process. Lastly, comprehensive patient education is crucial in empowering patients with the knowledge they need for management. It is crucial for patients to have an understanding of how to take care of their wounds, recognize any signs of complications and ensure they control their blood sugar levels. Therefore, when it comes to managing orthopedic complications in individuals with diabetes, such as Charcot foot diabetic neuropathy and surgical considerations a comprehensive and patient-focused approach is taken. Managing these complications effectively requires implementing a range of strategies that focus on relieving symptoms, preventing issues and improving health. It is crucial for healthcare professionals, from specialties, to collaborate and provide care to diabetic patients dealing with these intricate challenges.
Conclusion
It is crucial to take an approach when dealing with issues in patients with diabetes. This involves aspects such as providing support and immobilization for Charcot foot, managing blood sugar levels effectively addressing pain and ensuring careful perioperative care for any surgical interventions. The collaboration between healthcare professionals plays a role in achieving outcomes and enhancing the quality of life for diabetic patients who face these complex challenges. Early identification, timely intervention and patient education are factors in achieving success in managing these orthopedic complications associated with diabetes. Offering care through teams is essential to address these complex orthopedic challenges faced by individuals with diabetes.
Disclosure
Conflict of interest
There is no conflict of interest.
Funding
No funding
Ethical consideration
Non applicable
Data availability
Data that support the findings of this study are embedded within the manuscript.
Author contribution
All authors contributed to conceptualizing, data drafting, collection and final writing of the manuscript.