Volume 4, Issue 1
January 2024
An Overview of Hematologic Emergencies in Sickle Cell Anemia
Samar Alharbi, Eman Baothman, Abdullah Alharbi, Mohammed Alhadi, Khlood Alrowathi, Abdulaziz Alahmari, Abdulrahman AlQahtani, Osamah Alsuwilem, Umme Habiba Baqrain, Zainab Jaafar, Fatema Alnashaba
DOI: http://dx.doi.org/10.52533/JOHS.2024.40106
Keywords: Sickle Cell Anemia, Hematologic Emergencies, Vaso-Occlusive Crises, Transcranial Doppler Ultrasonography, Comprehensive Care Strategies
Sickle cell anemia (SCA) is a hematological disorder characterized by a form of hemoglobin called HbS. This results in the formation of rigid crescent-shaped red blood cells and various complications, including emergencies related to the blood. This literature review provides an overview of these emergencies, focusing on their signs, diagnostic methods, and current treatment approaches. The main feature of SCA, hemolysis, contributes to vaso-oclusive crises, where small blood vessels become blocked and cause tissue damage due to reduced blood flow. Early identification through parameters and advanced imaging techniques like magnetic resonance imaging plays a role in effective management. Acute chest syndrome, an emergency involving blocked lung blood vessels, requires recognition and aggressive treatment that includes oxygen therapy, pain relief measures, and transfusions if necessary. The increased risk of stroke in individuals with SCA necessitates detection using doppler ultrasonography, especially in pediatric patients who may benefit from long-term transfusion therapy for prevention purposes. Comprehensive care for SCA patients goes beyond managing crisis situations and includes vaccinations, genetic counseling services well, and patient education. Exciting advancements in SCA management, such as gene therapy, offer options for the future. The review highlights the importance of taking an approach to address emergencies in SCA, which involves leveraging clinical expertise conducting laboratory investigations, and exploring innovative therapies. As researchers delve deeper into the intricacies of this condition, the path to care keeps advancing in a direction. This progress brings optimism for outcomes and an improved quality of life.
Introduction
Sickle cell anemia (SCA) is a blood disorder characterized by the presence of hemoglobin called hemoglobin S (HbS) (1). This genetic mutation causes the formation of crescent-shaped blood cells, which can lead to various complications, including emergencies related to blood disorders. Managing hematologic emergencies, in SCA presents challenges. Requires a thorough understanding of the underlying pathophysiology. In this review, we aim to provide an overview of emergencies in sickle cell anemia, focusing on their clinical manifestations, diagnostic approaches, and current treatment strategies. Hemolysis, a defining feature of sickle cell anemia, plays a role in the development of emergencies. Intravascular hemolysis results in the release of hemoglobin leading to dysfunction and depletion of nitric oxide. These events contribute to vaso crises which are among the most common hematologic emergencies seen in SCA (2). Vaso occlusive crises are characterized by blockage of blood vessels, causing tissue damage and ischemia. The associated pain is often severe. Requires intervention. Numerous studies have highlighted the importance of diagnosis for managing vaso-occlusive crises (3, 4). Hematologic parameters such as levels of hemoglobin reticulocyte count and lactate dehydrogenase (LDH) can serve as indicators for assessing the severity of hemolysis and guiding treatments (5, 6). Furthermore, the progress made in imaging methods, like magnetic resonance imaging (MRI), has offered an understanding of the pathophysiology of vaso crises. This knowledge helps in identifying and managing them promptly and effectively (7, 8). Acute chest syndrome (ACS) is a blood disorder that requires attention in individuals with sickle cell anemia (SCA). ACS occurs when blood vessels in the lungs become blocked causing symptoms like chest pain, difficulty breathing, and low oxygen levels (9). Recognizing ACS and taking measures to prevent further deterioration and improve outcomes is crucial. The management of ACS primarily involves measures such as providing oxygen therapy, controlling pain and administering blood transfusions (10). People with SCA often face a risk of stroke due to their tendency to develop blood clots. Stroke in SCA can be caused by factors, including both small blood vessel abnormalities. Doppler (TCD) ultrasonography is a tool used to identify children at high risk of stroke so that early intervention through regular blood transfusions can be initiated to prevent recurrent events. Apart from vaso crises and stroke splenic sequestration is another hematologic emergency that primarily affects children with SCA (11, 12). This condition involves pooling of blood in the spleen leading to enlargement and potentially life threatening low blood volume shock. It is important to monitor spleen size and promptly administer blood transfusions as necessary to prevent complications associated with sequestration. Managing hematologic emergencies in individuals with SCA extends beyond interventions; comprehensive care strategies are essential, for preventing recurring crises (13). Hydroxyurea, a medication that helps modify diseases has shown effectiveness, in reducing the occurrence and intensity of vaso crises by promoting the production of hemoglobin. Moreover, breakthroughs in gene therapy offer hope, for a strategy to address the root problem in sickle cell anemia (14). Hematologic emergencies, in sickle cell anemia, present a range of challenges including vaso crises, acute chest syndrome and stroke. It is crucial to identify and manage these emergencies for patient outcomes. The use of tools like TCD ultrasonography and MRI along with research on innovative treatment methods shows progress in caring for individuals with sickle cell anemia (15). As we continue to understand the complexities of this blood disorder, a multidisciplinary approach that combines expertise, laboratory investigations and innovative therapies will play a role in reducing the impact of hematologic emergencies in sickle cell anemia. This review provides an overview of emergencies in sickle cell anemia.
Methodology
On December 4th, 2023 we conducted an analysis of articles, from the Cochrane Library, PubMed and Scopus. Their main objective was to gain an understanding of emergencies in individuals with sickle cell anemia. They systematically searched for information using keywords like "sickle cell anemia " " chest syndrome," and "complications." The articles they reviewed were written in English. Published since 2008. In addition to the text based content they also examined visuals such as an x ray that depicted acute chest syndrome. This comprehensive approach aimed to provide insights, into the complications associated with sickle cell anemia.
Discussion
The management of emergencies, in sickle cell anemia (SCA) requires a multifaceted approach. Vaso occlusive crises, which are a manifestation of SCA need prompt and personalized pain management strategies. The frontline interventions consist of opioids, nonsteroidal anti-inflammatory drugs (NSAIDs) and intravenous fluids. It is crucial to emphasize diagnosis by using parameters and advanced imaging techniques, which highlight the importance of proactive monitoring and intervention (16). Acute chest syndrome (ACS) another hematologic emergency demands a strategy that includes oxygen therapy, pain control and blood transfusions. Recognizing symptoms quickly and providing targeted interventions play a role in preventing the progression of ACS as it deals with life threatening complications related to pulmonary vaso occlusion. Given the increased risk of stroke among individuals, with SCA close monitoring and early intervention become necessary. Doppler (TCD) ultrasound is a tool, for identifying individuals at high risk enabling timely interventions like regular blood transfusions. Taking an approach to preventing strokes signifies a shift from managing crises to implementing strategies with the aim of improving long-term outcomes. The significance of monitoring and promptly intervening to prevent shock is underscored by splenic sequestration especially in pediatric populations. Timely blood transfusions play a role in avoiding complications associated with spleen enlargement highlighting the importance of an alert and proactive management approach. Hemolytic anemia in sickle cell disease (SCD) is closely linked to complications such as gallstones. Requires an approach. Addressing the relationship between hemolysis and its consequences treatment options include blood transfusions, hydroxyurea therapy and chelation therapy. A holistic approach to managing emergencies includes integrating care strategies such, as routine vaccinations and genetic counseling.
Clinical Manifestation
Hematologic emergencies, in sickle cell anemia (SCA) present a range of symptoms that are closely linked to the abnormal hemoglobin, vaso occlusive processes and inherent hemolysis that characterize this disease. Vaso occlusive crises (VOCs) are a hallmark causing intense pain due to the blockage of small blood vessels by sickled red blood cells. These painful episodes can affect organs and tissues requiring approaches to manage the pain based on triggers like infections, dehydration or exposure to cold temperatures (17). Another critical manifestation is chest syndrome (ACS) a life threatening condition caused by blockages in the blood vessels of the lungs (18) (Figure 1). ACS leads to symptoms such as chest pain, shortness of breath and low oxygen levels. Immediate attention is necessary with an approach addressing both lung compromise and potential infectious triggers.
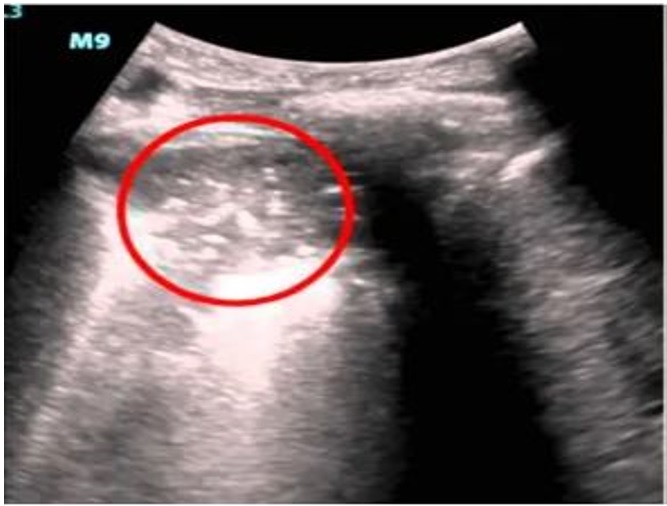
Figure 1: Sickle Cell Acute Chest Syndrome
The increased risk of stroke in SCA patients due to their state is particularly significant among patients and can result in focal neurologic deficits. Doppler (TCD) ultrasonography plays a role in identifying individuals at high risk for stroke allowing for early interventions such as chronic blood transfusions to prevent recurrent strokes (19, 20). Splenic sequestration is another complication seen in patients where there is sudden pooling of blood in the spleen leading to rapid enlargement and potential hypovolemic shock. Clinical signs include a spleen abdominal pain and indications of collapse. Timely recognition and prompt administration of blood transfusions are steps, in preventing complications. The widespread breakdown of blood cells, in sickle cell anemia leads to symptoms associated with anemia such as tiredness, paleness and difficulty breathing during activity. Laboratory markers like levels of hemoglobin counts of immature red blood cells and increased lactate dehydrogenase (LDH) levels highlight the presence of hemolysis. This chronic breakdown of blood cells also contributes to complications like the formation of gallstones due, to the buildup of bilirubin. Understanding the symptoms of hematologic emergencies in sickle cell anemia (SCA) is extremely important, for effective management. Healthcare professionals encounter a range of challenges from addressing the pain associated with vaso crises to dealing with complications like acute chest syndrome (ACS) stroke and splenic sequestration. It is crucial to recognize presentations and approach them from a multidisciplinary perspective in order to minimize the impact of these emergencies and improve the overall quality of life for individuals living with sickle cell anemia (Figure 2). Ongoing research provides insights and innovative therapies offering hope for advancements, in the care provided to patients with this challenging blood disorder.
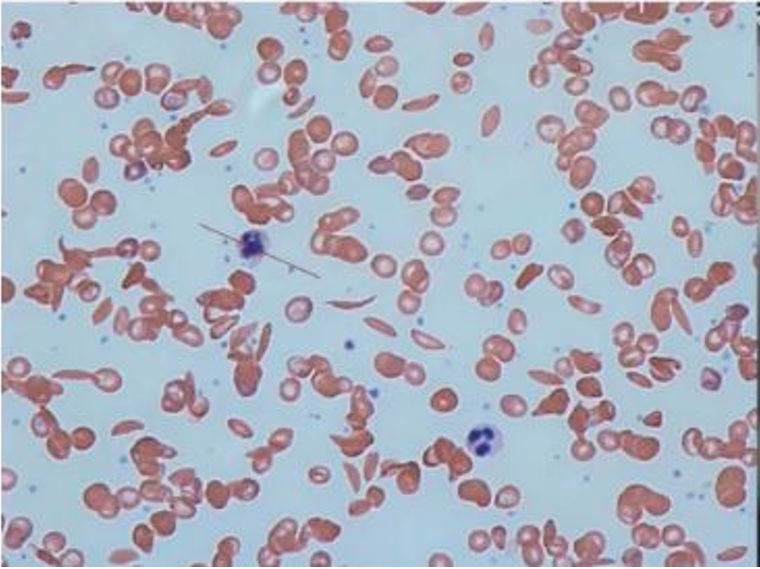
Figure 2: Sickle cell anemia in blood film
Management
Managing hematologic emergencies, in individuals with sickle cell anemia (SCA) requires a personalized approach due to the nature of these crises. It is crucial to have a strategy in place to address the clinical manifestations associated with vaso occlusive crises acute chest syndrome (ACS) stroke, splenic sequestration and hemolytic anemia. Vaso occlusive crises, characterized by pain and blockage of blood vessels require a multidimensional intervention. The main focus is on providing pain relief using opioids while also considering anti-inflammatory drugs (NSAIDs) as additional options. Intravenous fluid therapy plays a role in maintaining hydration levels and reducing the risk of dehydration, which can trigger vaso occlusive crises (21). In cases hospitalization may be necessary for intensive pain management and careful intravenous hydration. The management of ACS a life threatening condition caused by blood vessel blockage, in the lungs requires aggressive measures. We promptly start oxygen therapy to address levels of oxygen in the body and blood transfusions may be given to increase the amount of oxygen carried while reducing blockages, in blood vessels caused by sickle cell disease. We quickly introduce antibiotics to manage infections, bacterial pneumonia, which is a common trigger of acute chest syndrome (ACS). Managing pain and providing care including respiratory therapies are essential parts of ACS treatment. It is crucial to monitor for signs of difficulty breathing and intervene promptly to prevent complications. Due to the risk of stroke in individuals with sickle cell anemia (SCA) it is important to take steps for prevention (22). Transcranial Doppler (TCD) ultrasound plays a role in identifying high risk individuals on and guiding subsequent interventions. Regular blood transfusions can effectively reduce the likelihood of strokes by decreasing the amount of hemoglobin present. Additionally, hydroxyurea, a medication that modifies the disease process may also be considered for stroke prevention. Comprehensive care involves assessments TCD screenings and working closely with neurology specialists to optimize stroke prevention strategies. Swift intervention is necessary in cases where pediatric patients experience sequestration to prevent shock caused by blood volume. Immediate blood transfusions are given to relieve enlargement of the spleen and restore circulating blood volume. Regular monitoring of spleen size is crucial for intervention and follow up assessments are vital in evaluating the risk of recurrence. Collaboration with specialists is essential for management, in this population.
When it comes to dealing with anemia the key is to handle the hemolysis and its resulting complications. In cases of anemia and the accompanying symptoms blood transfusions may be required for management and relief. Hydroxyurea has shown effectiveness, in reducing hemolysis and the frequency of vaso crises by stimulating the production of hemoglobin. To manage iron overload resulting from transfusions chelation therapy might be necessary while folic acid supplementation is commonly prescribed to support the production of blood cells. In addition to crisis management comprehensive care involves monitoring of laboratory parameters. Vaccinations, against encapsulated bacteria are crucial for preventing infections in individuals with compromised systems. Genetic counseling is a part of care as it helps patients make informed decisions and adhere to prescribed treatments. Education initiatives targeting both patients and their families are essential for understanding and compliance with the management plan. Gene therapy has emerged as an avenue in the field of emerging therapies aiming to correct the underlying defect and potentially offer a curative approach. Ongoing research on targeted therapies and disease modifying agents holds promise for expanding treatment options and improving outcomes for individuals with sickle cell anemia (SCA). Encouraging participation in trials is not vital for advancing scientific knowledge but also critical for broadening the available treatments for managing hematologic emergencies in SCA. In conclusion managing emergencies, in sickle cell anemia requires a personalized strategy. Healthcare providers face the challenge of managing a range of situations from effectively controlling pain, during vaso occlusive crises, to preventing strokes, hypovolemic shock and complications associated with hemolytic anemia. It's a changing and intricate landscape that they navigate through. Progress, in treatments, combined with support and continued scientific investigation bring optimism for better results and an improved quality of life for those facing the complex difficulties of sickle cell anemia and its related blood disorders. The changing path of care demonstrates a dedication to meeting the requirements of individuals, with SCA through a progressive approach.
Conclusion
In conclusion effectively managing emergencies, in sickle cell anemia requires a dynamic strategy. The shift from crisis driven interventions to measures reflects advancements in diagnostic tools, treatment methods and a deeper understanding of the underlying causes. The incorporation of therapies like gene therapy shows potential for significantly improving the care provided to individuals with SCA. As healthcare professionals navigate this landscape it becomes essential to prioritize collaboration and continuous research. The approach to caring for SCA is progressing towards a patient centered and holistic paradigm that not focuses on resolving crises but also emphasizes the prevention of recurring emergencies. This looking approach, combined with advancements in treatment options positions the management of emergencies in SCA on a positive trajectory offering better outcomes and an enhanced quality of life, for individuals facing the challenges associated with this blood disorder.
Disclosure
Conflict of interest
There is no conflict of interest
Funding
No funding
Ethical consideration
Non applicable
Data availability
Data that support the findings of this study are embedded within the manuscript.
Author contribution
All authors contributed to conceptualizing, data drafting, collection and final writing of the manuscript.
