Volume 4, Issue 4
April 2024
Giant Congenital Melanocytic Nevi: A Case Report in Madinah, Saudi Arabia
Khulood Fallath, Mohammed Alharbi, Taif Tharwat, Ohoud Alahmadi, Lujain Khayat
DOI: http://dx.doi.org/10.52533/JOHS.2024.40402
Keywords: neonate, giant congenital melanocytic nevi, multidisciplinary management, malignant
Giant congenital melanocytic nevi (GCMN) is an uncommon disorder that impacts newborns, with a prevalence of less than 1 in 20,000 births. Even though it is uncommon, detecting the condition early is essential because of the higher chance of complications such as malignant melanoma, central nervous system involvement, and negative effects on the patient and their family's mental well-being due to its unattractive appearance. A giant congenital melanocytic nevus (GCMN) is described as a dark brown skin lesion acquired at birth that has the potential to grow to over 40 cm in size as a person reaches adulthood. The diagnosis of the GCMN is clinically confirmed, while management is mainly symptomatic. Nevertheless, treatment options could consist of surgical and non-surgical methods, psychological therapy, and/or regular clinical monitoring, taking into account alterations in color, size, texture, or the area of the lesion. We describe here a case of GCMN in a male neonate observed in our practice. The patient presented with a huge, pigmented patch over the body since birth, encompassing the entire abdomen, extending to the chest, thighs, and genitalia with multiple satellite, a few lesions on the face, and laterally towards the posterior aspect of the trunk, involving the entire back and buttocks. Radiological investigations were performed and were reported as normal with no significant findings. Additionally, the MRI also did not indicate any involvement of the central nervous system; hence, multidisciplinary comprehensive care was followed for this neonate with monthly regular follow-ups at dermatology and pediatric clinics. Our case significantly highlights the observatory interdisciplinary management of this condition; however, if needed in the future, surgical intervention maybe considered to decrease the risk of malignancy.
Introduction
Congenital melanocytic nevus (CMN) is a cutaneous lesion characterized by benign proliferations of nevomelanocytes (1). They can often be seen on the back and thigh with a brown to a black color appearing at birth or within the early weeks of life, However, limited research shows appearance as late as two years old (2, 3). Although small CMNs are frequently seen, giant congenital melanocytic nevus (GCMN) is uncommon in newborns. GCMN may manifest as single lesions or be accompanied by multiple, diffusely spread satellite nevi, in which case the term GCMN syndrome is applied, and they can reach up to 40 cm in size as a person reaches adulthood (4).
The incidence of CMN varies based on size with approximately one in 100 babies thought to have a tiny CMN, one in 1000 with a medium CMN, and one in 20,000 to one in 500,000 have a huge or enormous CMN (3, 5, 6). Notably, there appears to be a somewhat higher frequency of CMN in females compared to males, with a reported ratio of 3 to 2 (2).
The classification of CMN based on size is essential for risk stratification and management planning. CMNs are categorized as small, medium, huge, or enormous depending on the maximum diameter of the lesion's expected mature size. Generally, small CMNs have a diameter of less than 1.5 cm, medium CMNs range from 1.5 to 19.9 cm, while large/giant CMNs exceed 20 cm in diameter (7). The anatomical location of the nevus also influences its estimated adult size, with scaling factors applied to predict expansion. Larger lesions have a greater chance of melanoma, cosmetic implications, surgical challenges, and a greater incidence of related symptoms. However, it is worth noting that smaller nevi are rarely observed to progress to melanoma (8).
While smaller CMNs are regarded as rather frequent lesions, GCMNs are uncommon, despite the estimated incidence varying across research. Although it is uncommon, every patient with GCMN should be regarded as a suspect for the development of neurodermal melanosis, regardless of whether they exhibit neurological symptoms. Magnetic resonance imaging (MRI) of the brain and spinal marrow is recommended before brain myelination (9). Management options for GCMN include surgical excision, laser therapy, and other superficially destructive techniques, and conservative management with close observation (10). The decision-making process for selecting the most appropriate treatment strategy must take into account factors such as the size and location of the nevus, the patient's age and overall health, and the potential risks and benefits of intervention. Regardless of the chosen management approach, ongoing monitoring for melanoma risk remains paramount. Even after removal or treatment of GCMN, patients must undergo regular surveillance to detect any signs of malignant transformation.
Through the presentation of a case involving a large CMN in a male neonate, accompanied by a comprehensive review of the literature, we aim to contribute to the growing body of knowledge surrounding GCMNs. This case underscores the importance of early identification, multidisciplinary management, and ongoing research efforts to optimize the clinical management of this rare yet clinically significant condition.
Case Presentation
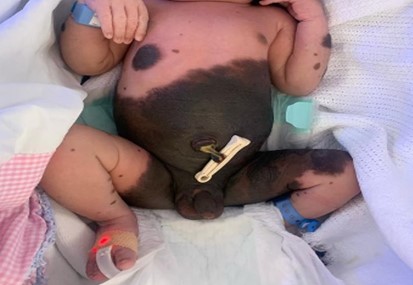
A male neonate, weighing 3 kg, was delivered through normal vaginal delivery to a multiparous mother. The antenatal history was uneventful. The neonate presented with a huge, pigmented patch over the body since birth, encompassing the entire abdomen, extending to the chest, thighs and genitalia with multiple satellite, few lesions on the face (Figure 1), and laterally spread towards the posterior aspect of the trunk, involving the entire back and buttocks. A large nodular lesion was observed in the back (Figure 2). There was no family history of a similar lesion.
The pigmented patch characterized by a dark brown to black with tufts of coarse and lusterless hair were dispersed across the lesion at the back and elsewhere. Further investigations included an MRI of the head, which showed no deep central nervous system extension. Ultrasound of the abdomen, X-ray of the spine, and fundus examination yielded normal results. The patient was enrolled in monthly follow-up examinations by a dermatologist and followed up by a pediatrician, ensuring a comprehensive and multidisciplinary approach to care.
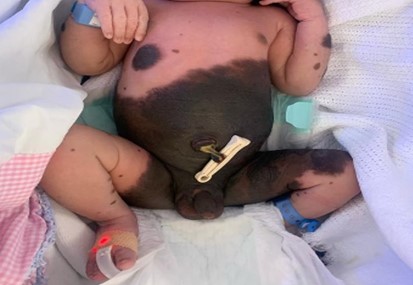
Figure 1: Multiple pigmented satellite lesions
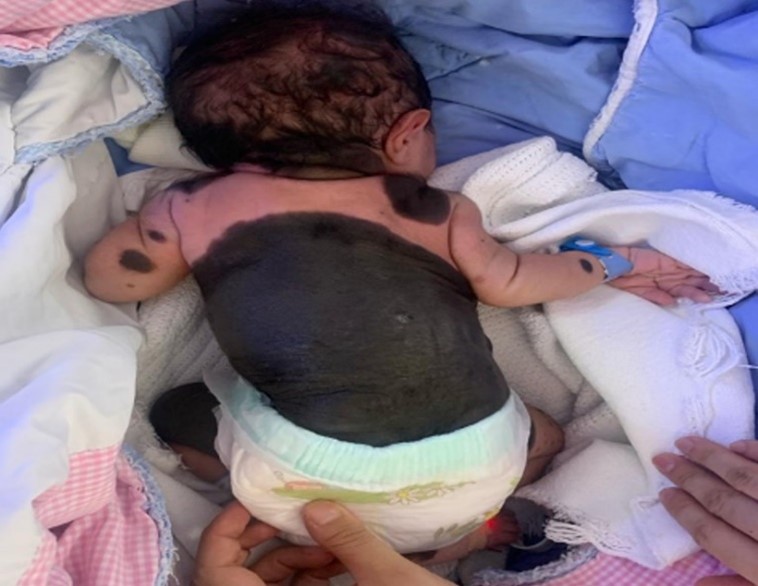
Figure 2: A large nodular lesion was observed in the back
Discussion
The pigmented cutaneous lesions in CMN are formed by nevus cells originating from both the dermis and the epidermis, and in case of excessive hair development, they are additionally referred to as big hairy nevi. Melanoblasts proliferate and migrate abnormally from the neural crest to the skin, mucosae, leptomeninges, mesentery, eyes, and ears, which results in the formation of CMN (2, 6). However, hepatocyte growth factor/scatter factor (HGF-SF) and other genetic abnormalities such as NRAS (Q61) and BRAF (V600) mutations might also lead to the development of this condition (11). In a culture of melanocytes from the nevus, chromosomal rearrangements involving 1p, 12p, and 19p have been observed. While evidence from one research study demonstrated that 21 individuals with CMN had 14 somatic mutations, and 57% of the lesions had NRAS gene alterations (12). A gain of function mutation in the NRAS gene linked to GCMN was discovered in another research, which eventually caused an aberrant proliferation of melanoblasts. A few of the case reports from the existing literature also suggest that the MAPK pathway is triggered by BRAF-activating mutations, which include single-nucleotide variations and fusions (13). Furthermore, some researchers have also evaluated the role of the protein HGF/SF in the dispersion and migration of neuroectodermal cells, leading to their presence throughout the body. Extra pigment and atypical skin cells described as nevus cells occur as a result of excess or aberrant protein in certain cells (2).
The most reliable method for diagnosing malignant melanoma is histopathology. With melanocytes that may penetrate even the muscle, glands, arterial walls, nerve tissues, and fasciae, it exhibits intradermal or complex involvement (13). Excisional biopsies are used to diagnose melanoma in GCMN patients, with punch biopsies being recommended for exposed areas such as the palms, face and soles (14). Its presence raises the risk of neurocutaneous melanosis and malignant melanoma, both of which have two common presentations: malignant degeneration or the emergence of extracutaneous melanocytes in the (central nervous system) CNS (15). A disorder called neurocutaneous melanosis occurs due to abnormal development of neuroectodermal cells, leading to uncontrolled growth of melanocytes in inappropriate areas such as the CNS (16). The probability of CNS involvement is increased by the occurrence of several satellite lesions and involvement of the head or trunk midline. Because of the timeline for myelination in the brain, using magnetic resonance imaging of the brain and spinal cord is considered the best method for diagnosing CNM. This imaging commonly occurs when the infant is between 4 and 6 months old (16). However, in our instance, imaging tests (echo and cardiac imaging which were normal) done few weeks after birth showed no involvement of the central nervous system or any related abnormalities, despite the large size and satellite distribution of the lesion. The main justification for removal is the CMN's development of malignancy; however, evidence for the research regarding the frequency of malignant transformation is limited. Different rates have been documented. After doing a retrospective analysis of the Netherlands' national pathology database, Zaal et al. found that the incidence rate of malignant melanoma was more than what would be predicted for the whole population (17). These patients are at a risk that is twelve times greater than that of the general population. In addition, women are more likely than males to get cancer (14.1 vs 6.4). Furthermore, with an incidence rate of 51.6, the research indicated that GCMN had an even greater risk of malignant melanoma. Consequently, it is essential to continuously examine these lesions to quickly identify any indications of malignant alterations. As in our case, routine follow-up examinations by pediatricians and dermatologists are crucial for early diagnosis and action, which reduces the likelihood of unfavorable consequences.
Additionally, a prospective study conducted by Viana et al, which involved all individuals with GCMN in the Giant Congenital Melanocytic Nevus Registry of Minas de Gerais Federal University, revealed that the lifetime incidence of malignant melanoma in these patients was approximately 5%. The study was carried out between 1999 and 2011 (18). Further, the authors suggested that they have a tendency to appear in central areas as the trunk was the most common location (68.4%), followed by the head and neck (17.5%), and lastly the extremities (14.1%). Satellite lesions were found in nearly 84.2% of patients with giant congenital melanocytic nevi (GCMN) and are associated with an increased risk of both cutaneous melanosis and malignant melanoma. Both Viana et al. and Zaal et al. recommend surgical removal to decrease the number of nevomelanocytic cells in order to reduce the risk of malignancy if the malignant transformation occurs within the nevus (17, 18). According to Krengel et al., a thorough examination of 14 studies with 49 cases of CMN melanoma revealed that 67% of patients had malignancy within the nevus, suggesting the need for preventive surgical removal (19). However, since in our case, the radiological investigations turned out normal, we opted for observatory interdisciplinary management of the patient presently.
Various treatment options, such as tissue expanders and partial and full-thickness skin grafts, have been suggested; however, each has drawbacks and restrictions. In research presented by Schiestl et al. (20), utilized Integra (Integra Artificial Skin) effectively as a replacement for all skin defects following complete nevus removal in the surgical treatment of GCMN (20). The two phases of treatment were, depending on the situation, partial or full-thickness skin grafts after the GCMN was excised and Integra was placed. The integration rates of the dermal matrix initially ranged from 95% to 100%. While there was a relatively high (33%) risk of complications, issues like loss of Integra or graft integration, and infections requiring removal of grafts were mild problems (21).
For the first three years of treatment, there will be a minimum yearly evaluation of the lesions, followed by a two- to five-year follow-up. According to published studies, surgery is the cornerstone of care for CMN (22). The decision for surgical excision is evaluated at six months of age, preferably after assessing neurological extension and CNS involvement, along with the issues of technical difficulties and uncertainty regarding effective prophylactic against the development of melanoma, even though it is impractical at initial presentation, especially for small lesions (9). Though leptomeningeal involvement will not completely reduce the risk of melanoma even after surgical excision, procedures employed in surgical therapy include repair with skin grafting, local rotation flaps, and serial excision (23). Partial GCMN removal has been achieved using skin curettage, dermabrasion, lasers, and chemical peels for both cosmetic and psychological reasons. The surgical therapy involves a series of excisions followed by rebuilding using free tissue transfer, local rotation flaps, skin grafting, and tissue expansion.
Conclusion
In conclusion, this case emphasizes the need for close observation and interdisciplinary teamwork in the treatment of gigantic CMN. Although the given neonate's lack of involvement of the central nervous system is encouraging, routine follow-up exams are necessary due to the possibility of neurocutaneous melanosis and malignant transformation. If the features of the lesion and the possible effect on the patient are carefully assessed, surgical intervention may be considered to reduce the risk of malignancy.
Disclosure
Conflict of interest
There is no conflict of interest.
Funding
No funding
Ethical consideration
A written informed consent was taken from the patient’s parents to include the data in the form of case publication with protection of the patient’s anonymity.
Data availability
Data that support the findings of this study are embedded within the manuscript.
Author contribution
All authors contributed to conceptualizing, clinical data drafting, diagnosis, treatment and final writing of the manuscript.